Introduction
About 70–80% of cancer patients experience nausea, vomiting, or both after chemotherapy.1 Although there are many antiemetic medications to alleviate chemotherapy-induced nausea and vomiting (CINV), such as serotonin (5-HT3) antagonists, antiemetic agents have noticeable side effects and cannot always provide satisfactory prevention of symptoms. Clinical use of 5-HT3 antagonists can control episodes of emesis to some extent; however, chemotherapy-induced vomiting is still a serious problem to overcome. Also, appetite loss is commonly reported by people receiving chemotherapy even among those who do not report nausea. It is unclear to what extent this relates to altered taste function or to changes to the sense of smell or touch. More than approximately half of chemotherapy patients experienced loss of appetite.2
Among alternative therapies, acupuncture is the technique that has been mainly assessed for its efficacy in controlling CINV. Several studies have investigated the efficacy of acupuncture in CINV3–9, with needles manipulated or electro-stimulated, and those studies adopted NeiGuan (P6) as the main acupoint for alleviating CINV, although some introduced other acupoints, such as Zusanli (ST36), Zhongwan (CV12), Hegu (LI4), Nei Ting (ST44), and Gong Sun (SP4).3,4,8 These acupoints were selected to treat CINV solely or in combination with P6.
A majority of clinicians use the combination of multiple acupoints, which may be more effective than a single acupoint for enhancing the therapeutic response. Particularly, SP4 is an acupoint employed to treat gastralgia, vomiting, abdominal pain, diarrhea, etc.10,11 and a previous study using the combination of P6 and SP4 with Bai Hui (DU20) reported an improvement in idiopathic refractory nausea.11
Methods
An observational study was conducted on twelve patients between January 2011 and December 2011 at the Daegu Catholic University Hospital of Korea. Acupuncture was started from 1st day of chemotherapy and applied at two acupoints, P6 and SP4, bilaterally with manipulation strong enough to generate De-Qi sensation. P6 is located on 2 cm above the transverse crease of the wrist, between the tendons of the muscularis palmaris longus and the flexor radialis. SP4 is located in the depression distal and inferior to the base of the first metatarsal bone. After 25 minutes of acupuncture, the needles were removed. Acupuncture was performed by government-registered traditional Korean medicine physicians with clinical careers of over 10 years. The needle types used were sterile, disposable, stainless steel needles (30 × 0.25 mm; Dongbang Acupuncture Inc., Chungcheongnam-do, Korea). The skin was swabbed with an alcohol prep pad before acupuncture was administered, and needles were inserted into the skin at a depth of 10–20 mm. The study involved 5 treatment sessions over 5 consecutive days, once a day, with a follow-up examination at 1 week after final treatment.
CINV was recorded as the visual analogue scale (VAS) score of nausea, anorexia and vomiting severity. All patients completed an open questionnaire for vomiting and nausea after each treatment session and 1-week follow-up. “Index of Nausea, Vomiting & Retching”, provided by Rhodes et al 12, was used to evaluate nausea and vomiting. The instrument consists of 8 questions with 5-point scale, possible score 0 [none] to 4 [severe]. Loss of appetite was evaluated by VAS score with scale of 0 [none] to 10 [severe]. At every treatment session, adverse events associated with acupuncture were recorded by investigators.
Results
12 cancer patients (7 men and 5 women) having underwent chemotherapy participated in this study, and they were aged between 49 and 68 years. The most common chemotherapy regimens included oxaliplatin (33.3%) and cisplatin (25.0%).
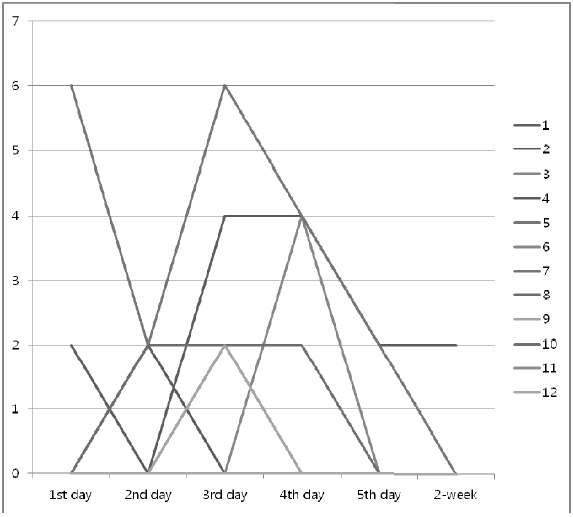
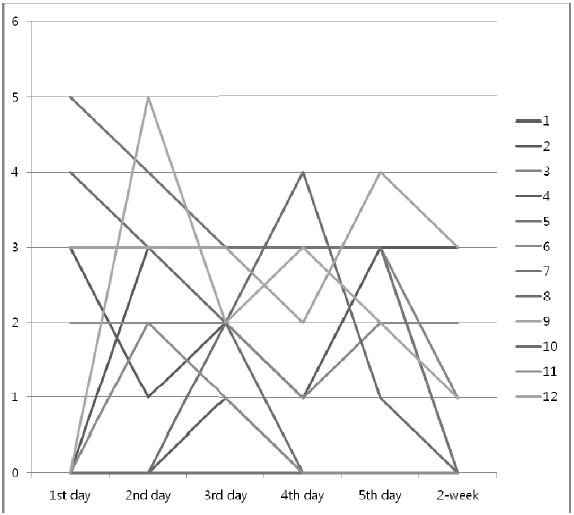
In total, 9 patients (75%) experienced CINV over time. Differences of CINV severity among patients’ characteristics are summarized in Table 1. The median Rhodex score showed 5 patients reported a decreasing pattern from Day 1 to Day 14, and 3 patients reported no CIVN. But, patients # 2, 6, 9 and 12, at Day 5, showed a higher severity than Day 1. In analysis of loss of appetite, 6 patients were improved over time, while other patients showed no improvement comparing the score at Day 1. Except for patient #3 and 6 there was no increase of loss of appetite between Day 5 and Day 14.
During the study, the mean of Rhodex of total patients revealed a decrease of Day 1, Day 7, Day 14; 0.74, 0.68, 0.38, respectively, while the mean of loss of appetite showed a decrease of Day 1, Day 7, Day 14; 5.25, 4.08, 4.00, respectively.
Discussion
The majority of studies investigating acupuncture in the control of CINV have used P6 as an acupoint, with a few also using ST36, ST44, and CV12 as additional acupoints. Each acupoint has its own therapeutic effect, and adjunctive acupoints are generally added to main acupoints for treating specific symptoms.13 Consequently, the coordination of acupoints may enhance the efficacy of acupuncture in controlling certain symptoms. According to traditional acupuncture theory, the combination of P6 and SP4 is used to treat diseases of heart, chest, and stomach, in particular, this combination is clinically used to treat gastric function disorder including nausea and vomiting. To our knowledge, until now there is no clinical study using this combination, except for one study10 investigating the effect of gastric function in rat model. Thus, to explore other acupoint candidates for the management of CINV, this study was performed by manual acupuncture of P6 and SP4.
Acute CINV occurs within 24 hours of chemotherapy, usually beginning within 2 to 4 hours and peaking in the first 4 to 6 hours, whereas delayed CINV occurs from day 2 to 6 of chemotherapy.14 In our study, we performed acupuncture during consecutive 5 days from first day following chemotherapy. Our study showed a lower severity at Day 5 than acute CINV (Day 1). One study reported that patients receiving chemotherapy experienced more delayed CINV twice than acute CINV.15
Loss of appetite induced by chemotherapy may be affected by various aspects such as fatigue, taste alternations as well as CINV. For instance, loss of eating pleasure as a result of a cisplatin-induced metallic taste is one examplet. A study performed by 24 sessions of acupuncture including P6 acupoint over 6 months showed a slightly decrease of loss of appetite.16 Loss of appetite is connected to weight loss and immunity in cancer patients, therefore, the investigation of the interventions for the enhancement of appetite need to be developed.
The current study was performed without concomitant administration of pharmacologic agents for emesis; however, previous studies using acupuncture plus antiemetics have shown that the combination was more effective than either acupuncture or antiemetics only.4,8 In addition, a recent randomized controlled trial including manual acupuncture of CV12, ST36, and LI4 revealed a positive effect of the treatment in alleviating CINV compared to placebo.7 Two other studies have also shown positive results for CINV.5,17 On the other hand, a randomized controlled trial with manual acupuncture of P6 revealed negative results in the prevention of acute emesis after chemotherapy versus placebo.6 These confusing results may be attributed to differences in the applied acupoints, sample sizes, or concomitant use of antiemetic drugs.
We observed the overall reduction of both CINV and loss of appetite, but there were differences of CINV severity among the patients. These results may be a preliminary data for a future study to confirm the affirmative effect of acupuncture on CINV, which should include a larger sample size with control group.