Customized BMI and waist circumference cut-off values are needed to identify metabolic syndrome among South Koreans according to their Sasang constitutional type
Article information
Abstract
Introduction
This study evaluated whether body mass index (BMI) and waist circumference (WC) cut-offs for predicting metabolic syndrome (MetS) were different according to Sasang constitutional type.
Methods
Data were obtained from 3,117 South Koreans (20–90 years old), and MetS was defined according to the revised NCEP-ATPIII criteria. Age-adjusted BMI and WC cut-offs were calculated according to Sasang constitutional type (Soyangin [SY], Taeeumin [TE], and Soeumin [SE]), sex, and age (men: ≥40 vs. <40 years, women: ≥50 vs. <50 years).
Results
The prevalences of MetS were 29.9% (<40-year-old men), 35.1% (≥40-year-old men), 14.8% (<50-year-old women), and 47.7% (≥50-year-old women). The BMI (kg/m2) and WC (cm) cut-offs for <40-year-old men were 25.9 and 89.9 (SY), 25.5 and 90.5 (TE), and 21.8 and 86.2 (SE). The cut-offs for ≥40-year-old men were 23.1 and 88.9 (SY), 25.0 and 89.9 (TE), and 22.2 and 87.5 (SE). The BMI and WC cut-offs for <50-year-old women were 22.5 and 81.2 (SY), 25.1 and 83.0 (TE), and 21.5 and 79.8 (SE). The cut-offs for ≥50-year-old women were 22.2 and 80.5 (SY), and 25.2 and 89.1 (TE), and 21.9 and 80.3 (SE).
Conclusions
The BMI and WC cut-offs for identifying MetS varied according to Sasang constitution type.
Introduction
Metabolic syndrome (MetS) is defined as a cluster of several components, which are hyperglycemia, dyslipidemia (i.e., elevated triglycerides and/or low high-density lipoprotein cholesterol), hypertension, and abdominal obesity1),2). The presence of MetS is strongly associated with the development of diabetes mellitus, cardiovascular heart disease, and increased mortality3). Thus, early-stage detection of MetS and subsequent follow-up are guided using various anthropometric indices, including body mass index (BMI), waist circumference (WC), and waist-to-hip ratio4),5). For example, abdominal obesity is determined using WC and is one of the most important factors for diagnosing MetS. In addition, a recent cohort study revealed that WC and BMI could help predict the development of diabetes6). However, the cut-off values vary according to sex and race, which suggests that anthropometric indexes for identifying MetS risk should be categorized according to sex, age, and/or race.
Sasang constitutional (SC) medicine is a holistic typological constitution medicine that is tailored to the Korean population and helps individuals balance their psychological, social, and physical aspects to achieve wellness and increase longevity7). This form of medicine classifies humans into four constitutions based on their traits: Taeyangin (TY type), Soyangin (SY type), Taeeumin (TE type), and Soeumin (SE type)8). Thus, it is possible that differences in clinical indexes (including body measurements) may be observed according to SC type, which may influence the assessment of health status9), and several studies have indicated that differences in pathological indexes can be observed according to SC type10–12).
Personalized medicine involves using accurate cut-off values to assess the patient (e.g., using WC and BMI to predict MetS) and select appropriate lifestyle modifications and/or treatments. However, it is difficult to determine individual cut-off values, which indicates that SC type could be a useful grouping, as differences in body shape, appearance, temperament, and physio-pathological symptoms can be observed according to SC type13). For example, the TE type is characterized by unique physiological patterns, hyperactive liver function, and hypoactive lung function, which reflects a state of weak consumption and strong storage of qi and body fluid14). In addition, the TY type is characterized by relatively large values for WC and BMI15). Recent studies have indicated that the TE type is an independent risk factor for various chronic disease, including diabetes, hypertension, and abdominal obesity16–18). Therefore, the present study aimed to identify the optimal WC and BMI cut-off values for predicting MetS according to sex, age group, and SC type among South Korean people.
Methods
1. Subjects
This retrospective study evaluated data from the Korean Medicine Data Center (KDC), which is part of the Korea Institute of Oriental Medicine (KIOM). The KDC maintains an integrated Korean medical database that was established in 2006 and is used for research purposes because it includes nationally representative clinical questionnaire, measurement, and biological data from Korean individuals who were assessed at multiple centers. Data were collected from November 2006 to July 2013, and subjects were considered eligible if they were 20–90 years old, although subjects were excluded if they could not understand or follow the researcher’s instructions, could not maintain proper posture during the measurements, if they were pregnant, or if they had body deformations (e.g., lumps or congenital malformations)18),19). The present study’s retrospective protocol was approved by the KIOM ethics review board (I-0910/02-001).
2. Sasang constitutional diagnosis
The SC diagnoses were performed by an expert in SC medicine at each hospital. These experts had >5 years of experience in clinical practice, and based their decisions on the subject’s physical body shape, facial appearance, temperament, and physical and/or pathological symptoms. Constitution-specific herbal formulae were administered according to the subject’s SC type, and only subjects who experienced a good response (i.e., clinical improvement without any adverse events) after >30 days of treatment were included. Previous studies have used the same procedures for diagnosing SC type9),20).
3. Data collection
Data regarding age, sex, weight, height, WC, blood pressure, and blood test results were collected to determine if MetS was present. WC was measured at the umbilicus level during a light exhalation while the subject was standing with their arms folded in front of their chest. Blood pressure was measured at each subject’s left upper arm after sufficient rest. Blood samples were obtained from the subjects’ left or right brachial veins after a ≥12-h fast, and were subjected to testing for fasting blood glucose, triglycerides, and high-density lipoprotein cholesterol. All laboratory tests were performed at a central laboratory to minimize test variability and error. Measurement bias was minimized by having an anthropometric measurement expert with 9 years of experience provide training to the examiners at least once per year. The KIOM monitored all data collection procedures and the examiners followed a standard operation procedure that was developed for the “Korea Constitution Multicenter Study”21).
4. Diagnostic criteria of MetS
MetS was defined according to the National Cholesterol Education Program Adult Treatment Panel III guidelines, which require the presence of at least 3 of 5 criteria22). The first four criteria were (1) diastolic blood pressure of ≥90 mmHg, systolic blood pressure of ≥140 mmHg, or receiving medication to treat hypertension, (2) fasting plasma glucose of ≥126 mg/dL or receiving medication to treat diabetes mellitus, (3) triglycerides of ≥150 mg/dL, and (4) high-density lipoprotein cholesterol of <40 mg/dL for men or <50 mg/dL for women. The fifth criterion was modified based on the WC cut-off values for abdominal obesity among Asian-Pacific populations (≥90 cm for men and ≥80 cm for women)23), as the MetS guidelines recommend cut-off values of >102 cm (40 in) for men and >88 cm (35 in) for women.
5. Statistical analysis
There are four SC types (TY, SY, TE, and SE), although the TY type was excluded because this type is too rare to perform accurate statistical analysis. One-way analysis of variance was used to evaluate continuous variables and the chi-square test was used to compare the prevalence of MetS among the three SC types. Receiver operating characteristic (ROC) curve analysis was used to determine the BMI and WC cut-off values for predicting MetS according to sex, age, and SC type. The age groups were selected based on menopause among women (<50 years vs. ≥50 years)24) and andropause among men (<40 years vs. ≥40 years)25). Data were analyzed using R software (version x64 3.4.1), and P-values of <0.05 were considered statistically significant.
Results
1. Anthropometric and clinical variables according to SC type
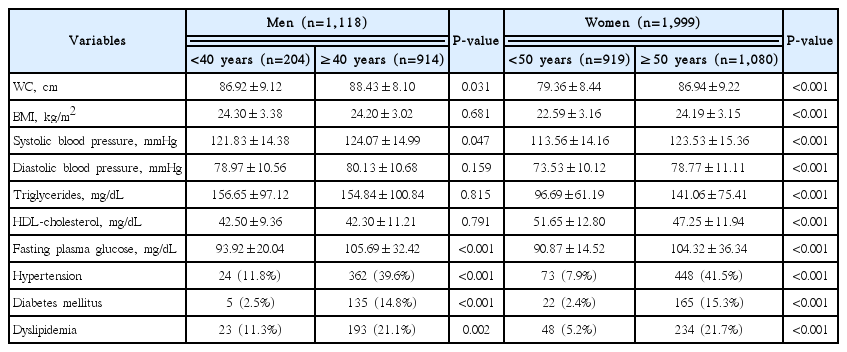
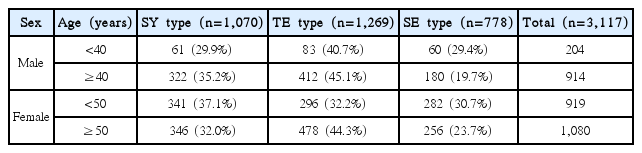
We detected significant differences in all anthropometric and clinical variables when comparing the two age groups of women, (Table 1), as well as in six of the ten variables on comparing the two age groups of men. The distribution of SC types is shown in Table 2: 1,070 subjects (34.3%) had the SY type, 1,269 subjects (40.7%) had the TE type, and 778 subjects (25.0%) had the SE type.
2. Prevalence of MetS and metabolic components according to sex
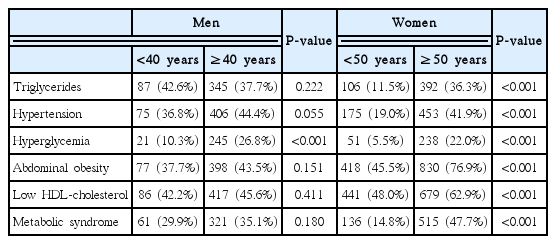
The prevalences of MetS were 29.9%, 35.1%, 14.8%, and 47.7% among <40-year-old men, ≥40-year-old men, <50-year-old women, and among ≥50-year-old women, respectively (Table 3). When we compared the two groups of men, the only significant difference was observed in the prevalence of hyperglycemia. However, all five components and MetS were significantly different between the two age groups of women.
3. ROC curve analysis
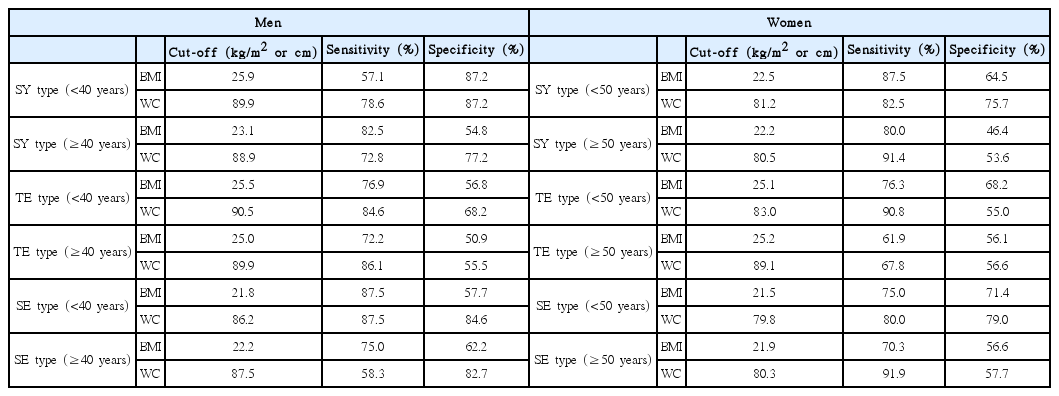
Figures 1 and 2 show the optimal cut-off values for BMI and WC according to sex and SC type. The sensitivity and specificity values for the BMI and WC cut-off values are shown in Table 4.
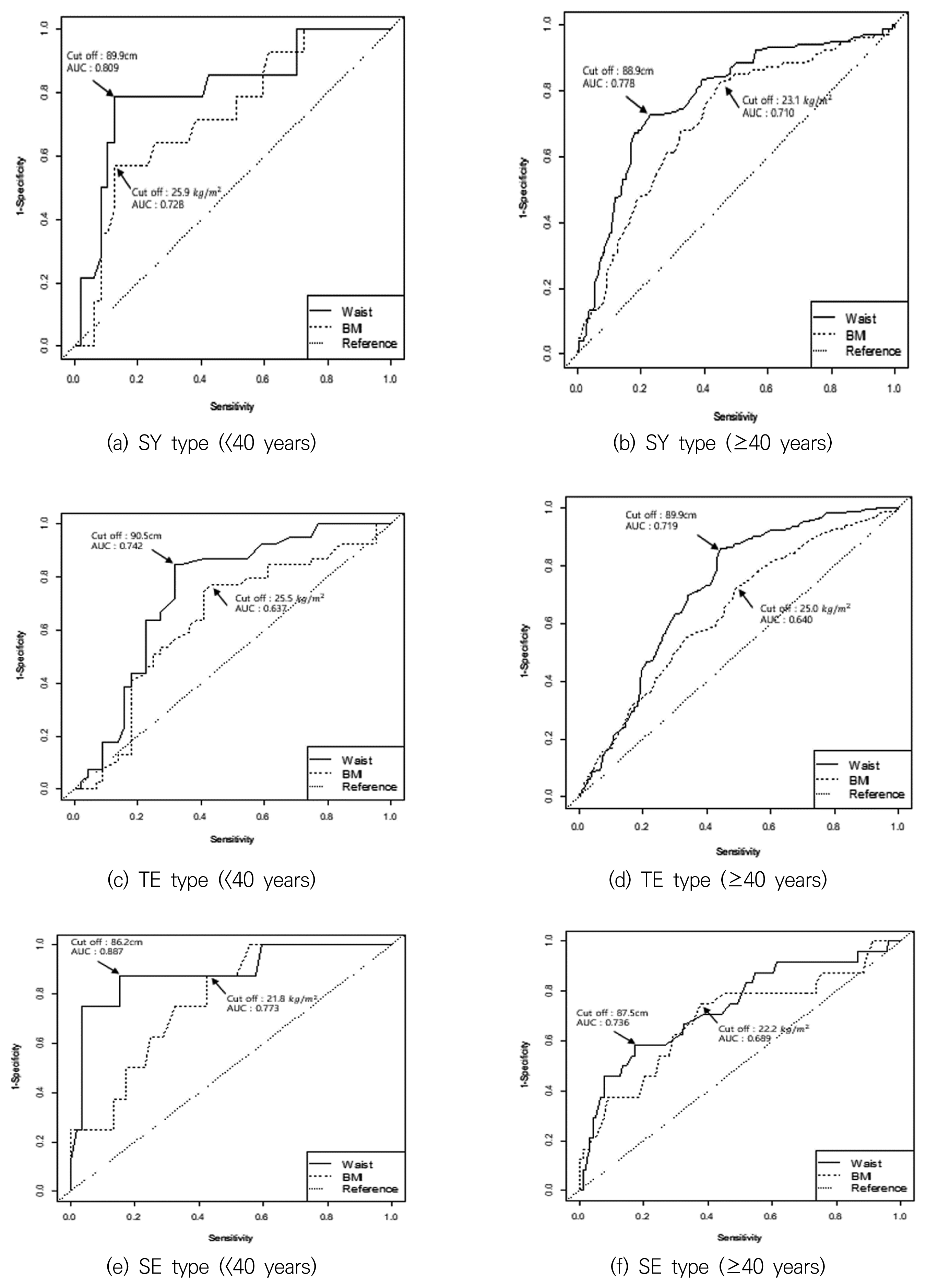
The cut-off values for waist circumference (Waist) and body mass index (BMI) according to Sasang constitutional type among men. SY: Soyangin, TE: Taeeumin, SE: Soeumin
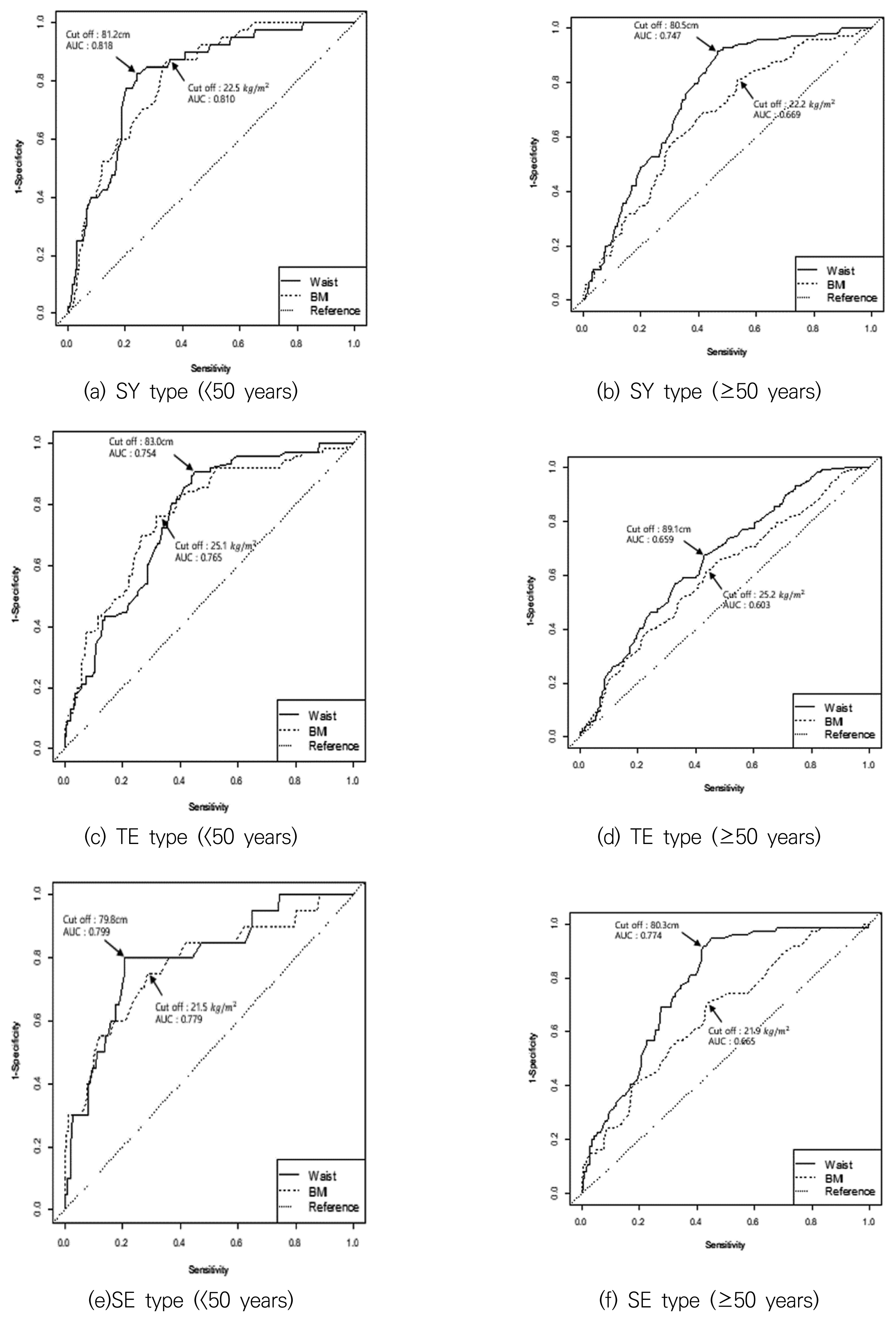
The cut-off values for waist circumference (Waist) and body mass index (BMI) according to Sasang constitutional type among women. SY: Soyangin, TE: Taeeumin, SE: Soeumin
Discussion
Recent studies of Western and traditional medicine have increasingly focused on personalized physical and genetic evaluations to predict the development of MetS16),26),27). Thus, the present study aimed to determine SC type-specific cut-off values for BMI and WC to predict the development of MetS. Furthermore, we assumed that aging-related physical changes could influence these cut-off values, and performed age- and sex-based analyses to determine more accurate cut-off values. The age-based analyses were performed using a cut-off age of 40 years for men (i.e., the approximate onset of andropause)25) and a cut-off age of 50 years form women (i.e., the approximate onset of menopause)24).
Groups with higher anthropometric values are generally thought to have a higher risk of MetS, compared to groups with lower values. For example, BMI has the highest ORs among TE-type women and WC has the highest ORs among non-TE-type women, while WC has the highest ORs in both TE-type and non-TE-type men. These results indicate that the predictors of MetS can vary according to SC type, and although WC is a good general predictor, BMI is superior when evaluating TE-type women9). Furthermore, one Korean study has also suggested that the appropriate WC cut-off values might be 90 cm for men and 85 cm for women28). Although BMI is not a MetS component, it is a convenient and applicable index. Thus, we identified SC type-specific cut-off values for WC and BMI according to age and sex group.
The present study revealed that, among men, the BMI cut-off values were 25.9 kg/m2 for the SY type and 25.5 kg/m2 for the TE type, which indicates that the standard cut-off (25 kg/m2) could be acceptable for these SC types. However, the cut-off value for <40-year-old men with the SE type was 21.8 kg/m2, which might indicate that the cut-off for this group should be lowered to 22 kg/m2. Furthermore, at ages of ≥40 years, the cut-off values were 23.1 kg/m2 for the SY type, 25.0 kg/m2 for the TE type, and 22.2 kg/m2 for the SE type, which may indicate that 23 kg/m2 is a more appropriate cut-off value for older men with the SY and SE types. The WC cut-off values among <40-year-old men were 89.9 cm for the SY type, 90.5 cm for the TE type, and 86.2 cm for the SE type, which may indicate that 90 cm is appropriate for the SY and TE types, although the cut-off should likely be lowered to 87 cm for <40-year-old men with the SE type. At ages of ≥40 years, the cut-off values were 88.9 cm for the SY type, 89.9 cm for the TE type, and 87.5 cm for the SE type, which also indicates that the cut-off value for ≥40-year-old men with the SE type should be lowered to 88 cm.
Among <50-year-old women, the BMI cut-off values were 22.5 kg/m2 for the SY type, 25.1 kg/m2 for the TE type, and 21.5 kg/m2 for the SE type. Thus, the cut-offs for the SY and SE types should be lowered to 23 kg/m2. Among ≥50-year-old women, the cut-off values were 22.2 kg/m2 for the SY type, 25.2 kg/m2 for the TE type, and 21.9 kg/m2 for the SE type, which indicates that the cut-off values for the SY and SE types should also be lowered to 23 kg/m2. Among the <50-year-old women, the WC cut-off values were 81.2 cm for the SY type, 83.0 cm for the TE type, and 79.8 cm for the SE type, which generally agree with the 80-cm cut-off value from the Asian-Pacific guidelines. Similarly, the cut-off values among ≥ 50-year-old women were 80.5 cm for the SY type, 89.1 cm for the TE type, and 80.3 cm for the SE type, which indicates that the cut-off value from the Asian-Pacific guideline is appropriate for the SY and SE types.
Interestingly, the WC cut-off value for the TE type was relatively high (89.1 cm), which indicates that women with the TE type became relatively obese as they experienced menopause. This conclusion is supported by the fact that the mean WC value among all ≥50-year-old women was 86.94±9.22 cm, compared to 79.36±8.44 cm among <50-year-old women. In addition, older women had a significantly high rate of MetS (≥50 years: 47.7% vs. <50 years: 14.8%), and older women with the TE type had the highest rate of MetS among all SC types (Table 2). In this context, the TE type seems to increase susceptibility to obesity because of a sensitivity to energy intake, based on an imbalance toward preserving energy, and physical differences are observed for each of the SC types29)]. Furthermore, a previous study revealed that the prevalence of MetS was 56.3%, 49.1%, 27.4%, and 26.4% among the TE-type men, TE-type women, non-TE-type men, and non-TE-type women, respectively9). Moreover, the TE type is prone to obesity30) and recent studies have revealed that the TE type is a risk factor for chronic diseases18), with TE-type women being prone to develop MetS as they experience menopause. Therefore, these women require careful monitoring and evaluation, and our WC cut-off value (89.1 cm) requires careful consideration in this group.
To the best of our knowledge, this is the first study to identify BMI and WC cut-off values for predicting MetS according to SC type, sex, and age group. One previous study has examined cut-off values according to SC type, and reported cut-off values for WC among TE-type men (89.9 cm), non-TE-type men (88.6 cm), and non-TE-type women (80.6 cm), as well as a BMI cut-off value of 25.2 kg/m2 among TE-type women9). However, the findings of the present study are more comprehensive, and may be useful for developing personalized management strategies. Furthermore, we attempted to increase the reliability of our findings by examining data from a Korean national database, which had implemented methods to minimize measurement errors using education and standard operating procedures.
The present study has several limitations. First, the study used a cross-sectional design, and the associations that we observed may not be causal. Second, body shape can be related to environmental factors, such as exercise and eating habits, although we were not able to evaluate these factors. Therefore, larger prospective studies are needed to validate our findings and determine the abilities of the WC and BMI cut-off values for predicting the development of MetS among individuals with each SC type.
Conclusion
The present study revealed that the WC and BMI cut-off values should likely be lowered for some groups of men and women with the SY and SE types. A higher WC cut-off value may be appropriate for older women with the TE type. The use of appropriate BMI and WC cut-off values may help more accurately predict the development of MetS according to SC type.
Acknowledgements
This research was supported by a “Establishment of Korean Medicine Genome and Epidemiology Infrastructure” grant from the Korea Institution of Oriental Medicine (K17091). The data supporting this study’s findings are available from the Korean Medicine Data Center (http://kdc.kiom.re.kr), although they are not freely available. Researchers who fulfill the criteria for access to confidential data can apply for access to the Korean Medicine Data Center. This research was funded by Sangji University 2016.
Notes
Conflicts of Interest
The authors declare that there are no conflicts of interest regarding the publication of this article.